Periodontitis: Symptoms, Home Remedies, & Treatments
The American Dental Association recommends you brush your teeth twice a day… And floss every day… And use mouthwash.
If we’re being honest, most people don’t keep up with this regimen every single day. That is probably why almost half of American adults live with gum disease, AKA periodontitis.
That is the reason I wanted to discuss the stages of gum disease, how to recognize the signs, and how to treat or even prevent it.
For instance, did you know there are toothbrushes that clean your teeth from multiple angles using multiple brush heads — and that these may be exactly what your gums need? Or, are you aware that fruit juice and sodas can be worse for your teeth than coffee?
What is gum disease?
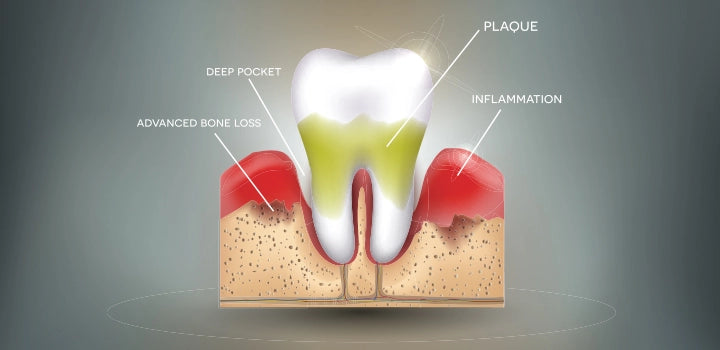
Simply put, it is inflammation of the gums. The first stage of gum disease is the more commonly heard of: gingivitis.
One way a dentist tests if you have gum disease is your pocket depth measurement. Using a periodontal probe and gentle pressure, your dentist will measure the depth of the pockets around each tooth. Healthy gum measurements range from 1-3 millimeters.
More than three millimeters, and you probably have periodontitis. That’s because the bacteria have eroded your periodontal ligaments, slowly separating your gums from your teeth.
Nearly half of all American adults have periodontal disease.
If periodontitis goes untreated, your teeth and alveolar bone (where your teeth are anchored) can take on a lot of damage. Fortunately, good oral hygiene practices can prevent gum disease and tooth damage and even stop existing periodontitis in its tracks.
Stages & Types of Gum Disease
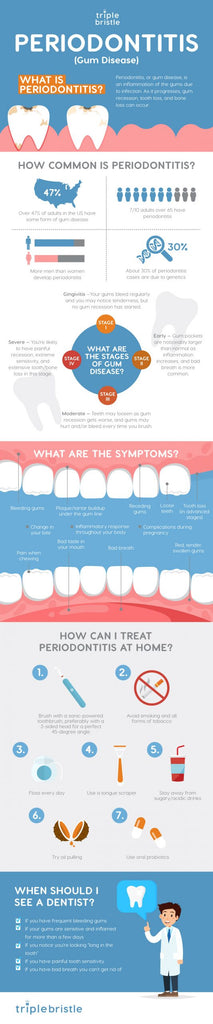
What are the four stages of gum disease?
- Stage I: Gingivitis
- Stage II: Early Periodontitis
- Stage III: Moderate Periodontitis
- Stage IV: Advanced Periodontitis
1. Stage I: Gingivitis
Gingivitis is an inflammation of the gums, and the first stage ofgum disease.
Bacteria build up forms plaque. Without proper cleaning, plaque buildup turns into tartar that only a professional can clean.
At this stage, the gums around your teeth will have a probing depth of 2-4 millimeters. You will experience no bone loss and no connective tissue loss.
But this bacterial invasion demands your attention. It is the mildest form of gum disease, but that means it is the most treatable. Reversing the inflammation of gingivitis can prevent the advancing of this disease.
While you are still in the first stage, take the opportunity to reverse your gum disease with good oral hygiene practices.
2. Stage II: Early Periodontal Disease
Early and moderate periodontitis are similar, but this is when more permanent damage may start to happen.
Your breath starts to worsen at this stage. Your gums recede. Your gums bleed more easily than ever when you brush your teeth.
Pocket depth measurements at the stage will be 4-5 millimeters. Your gums are disconnecting from your teeth. That is good for the bacteria looking for a place to hide away, but not good for you.
3. Stage III: Moderate Periodontal Disease
Similar to early periodontitis, moderate periodontal disease describes the stage at which gums are increasingly red and inflamed.
Breath gets even worse and harder to cover up. Gums will bleed very easily whenever you brush your teeth. You can experience some bone loss, and your teeth may loosen.
Moderate gum disease can trigger an inflammatory response in your whole body, and is generally when you may see other health concerns crop up (outside of the mouth).
Pocket depth measurements will be 6-7 millimeters. If the dentist is able to gently probe seven millimeters into your gums, you have a real problem.
4. Stage IV: Advanced Periodontal Disease
You will not be able to treat advanced periodontal disease at home. By stage IV periodontitis, you can expect to see bone loss of up to 50%. Your connective tissue deteriorates, and your teeth loosen even more.
By this stage, bacteria has invaded your gums and is actively, regularly transferred into your bloodstream. This messes with your immune system and triggers or worsens seemingly unrelated health problems.
Extreme pain while chewing, severe bad breath, tooth loss — if you have made it to advanced periodontitis, you should expect some severe symptoms.
Pocket depth measurement gets to be greater than 7 millimeters and gum recession is rampant at this stage. Your tooth roots may even be exposed, leading to painful tooth sensitivity.
Symptoms of Periodontitis
What are the early warning signs of periodontal disease? The symptoms of periodontitis and common complications generally include the following:
- When your gums bleed upon brushing or flossing
- Buildup of plaque or tartar on the surface of your teeth, under the gum line
- Bad breath
- Bad taste in your mouth (sometimes “metallic” tasting)
- Change in your bite
- Receding gums
- Red, tender, swollen gums
- Pain when chewing
- Inflammatory response throughout your body
- Loose teeth
- Higher risk of heart disease, respiratory disease, or diabetes
- Complications during pregnancy, such as low birth weight, premature birth, and preeclampsia
- Tooth loss (in advanced stages)
Since the symptoms of early periodontitis are not very noticeable, your dentist may be the first to point them out if you are not looking for them. However, a good rule of thumb is to immediately address any bleeding gums during brushing and flossing (gingivitis) and talk to your dentist if it happens more than very occasionally.
If not treated, periodontitis deteriorates the supporting structures of your teeth, like your jawbone and alveolar bone. Your teeth may loosen and fall out. A dentist may even need to extract the teeth.
Periodontitis Causes & Risk Factors
There are several possible causes of periodontitis. Here are the risk factors for periodontitis:
- Use of tobacco products, smoking
- Poor nutrition, especially a vitamin C deficiency
- Type 2 diabetes
- Obesity
- HIV infection
- Hormonal changes (such as menopause, pregnancy, menstruation)
- Leukemia
- Saliva-reducing medications
- Genetics
- Most importantly, poor oral hygiene
Also, lower income families are statistically more likely to develop gum disease. This is an unfortunate statistic, considering how expensive treatment can be for advanced periodontitis.
When you don’t brush your teeth every day or you don’t clean those hard-to-reach areas in your mouth, periodontitis can begin to surface.
Here is the process of how poor dental hygiene causes gum disease:
- Bacteria build up and multiply in your mouth. This gives way to dental plaque forming on your teeth.
- Without brushing, bacteria is able to deposit minerals in the plaque, turning the plaque into harder-to-get-of tartar.
- It becomes a vicious cycle, where the more tartar you have, the easier it is for tartar to develop.
- Your immune system tries to fight the bacteria, and your gums are inflamed.
- This inflammation leads to the gums separating from the teeth very gradually. This forms periodontal pockets where bacteria like to hide from toothbrushes.
- These bacteria release toxins that damage your teeth, gums, and supporting bone structure. This is when teeth may loosen and may even fall out.
Home Remedies
Can you fix periodontal disease? Why yes, you can fix periodontitis. If it has not progressed too far, better oral hygiene practices can reverse gum disease.
If it has advanced, you may need to see a dental professional, but we will talk about that in a little bit. First, I want to discuss home remedies.
How to Brush Just Right
Do not be scared of brushing the right way. Brushing your teeth well takes just a little bit of thought.
- Aim your toothbrush at a 45 degree angle, pointed towards your gum line.
- Brush in a gentle circular motion, not straight back and forth.
- You only need a pea-sized amount of toothpaste.
- Brush for at leasttwo minutes, with a traditional toothbrush.
- Use an electric toothbrush, preferably one with sonic technology.
Sonic Toothbrush
Because of the way a sonic toothbrush (one type of electric toothbrush) can break up plaque in open gum pockets, a sonic toothbrush is preferable to a traditional toothbrush.
Technically, a human should be able to operate a manual toothbrush so effectively that it is as good at removing plaque as a sonic toothbrush. But we are talking about a perfect human with powerful and precise muscles in their fingers, hands, wrist, and arm.
It’s best to stick with a sonic toothbrush, motioning in gentle circles at a 45 degree angle.
Don’t Smoke, Don’t Chew
Tobacco users are 3-6 times more likely to develop gum disease.
Tobacco is horriblefor your oral hygiene. Here are just a few reasons:
- Tobacco affects the saliva in your mouth, making it easier for bacteria to cling onto teeth and gums.
- About 90% of patients with mouth, throat, or lip cancer use tobacco products.
- Because tobacco inflames gum tissue, bacterial infections are more likely.
- Also, tobacco interferes with the blood flow in your gums, meaning gums take longer to heal.
- Tobacco stains your teethyellow.
Flossing (and not lying about it)
It’s wise to floss at least once every day. Floss can get rid of plaque buildup a toothbrush has trouble addressing.
Flossing before you brush has about as many benefits as flossing after. As long as you maintain both habits, your teeth will thank you.
And yet, only a third of adults floss.
According to a survey from the American Academy of Periodontology, more than a third of Americans would rather do an unpleasant activity than floss their teeth, such as sit in standstill traffic, do taxes, or scratch a chalkboard.
And about one third of American adults lie to their dentist about how much they floss. (Which is pointless, since your dentist can tell when you use dental floss.)
Surprisingly, flossing can clean up to 35% of your teeth that toothbrushes don’t reach.
Tongue Scraping
Tongue scraping is just what it sounds like. It is a quick way to get rid of unwanted particles loitering on your tongue — including bad breath-causing bacteria.
This is most effectively achieved with a small and slightly rounded device made of metal or plastic.
These advantages of tongue scraping may surprise you:
- Can improve sense of taste
- Can improve the appearance of your tongue
- Get rid of bacteria buildup
- Can improve bad breath
Avoid Sugar and Sugary Drinks
The worst drinks for your teeth are sugary drinks. Whether it be soda pop or fruit juice, sugary drinks feed and strengthen harmful bacteria that live in your mouth. Though indirectly, sugary drinks lead to more plaque and more risk of gum disease.
Many sugary drinks also contain acids that erode your teeth.
Though coffee can stain teeth, only sweetened coffee is truly bad for your long-term dental care.
Oil Pulling
Coconut oil is everywhere — in health, beauty, cooking, cleaning products. But coconut oil is useful for dental health as well.
Oil pulling is the all-natural method of swishing coconut oil (or sesame oil) around your mouth, which gets rid of bacteria and toxins. Instead of using mouthwash, which disrupts the balance of bacteria your mouth needs to stay healthy, oil pulling has been scientifically proven to reduce inflammation without hurting the oral microbiome.
The science behind coconut oil pulling is surprisingly forthright in how beneficial it can be. Oil pulling may prevent cavities, remove bad bacteria, reduce gingivitis inflammation, get rid of bad breath, whiten teeth, and promote general health.
You can oil pull daily or a couple times a week. Here are some easy steps:
- Before eating or drinking in the morning (water is fine), put a teaspoon or two of organic coconut oil into your mouth. If it’s solid, it will melt in your mouth — no problem.
- Swish the oil around like a mouthwash for about a minute.
- The oil will thicken over time, a result of mixing with saliva. If it is too much oil, adjust for next time.
- Because coconut oil is a solid below 76 degrees, it is best to spit out your swished coconut oil in the garbage can, not down the sink.
- Then, rinse out your mouth using warm water.
- Brush and floss your teeth as normal.
Oral Probiotics
You may have heard that probiotics were good for your gut. They are. Because your gut needs a good balance of good bacteria. And that’s what probiotics are — good bacteria.
We’ve discussed a lot about how bacteria in your mouth cause periodontitis. Well, if you take an oral probiotic, this seems to balance the good bacteria in your mouth.
A 2017 paper published in Dentistry Journal revealed oral probiotics do not cause any adverse side effects at all. It’s telling that the authors of this paper were very excited about the future of oral probiotics in treating or preventing dental and oral disease.
These chewables are most beneficial for correcting a “dysbiosis” (imbalance of bacteria) within the mouth once it’s started. That means they’re ideal for people with gum disease, as this inflammatory response is closely related to how healthy your oral microbiome is.
Why The Right Brush Is Your Best Defense
I already mentioned that a sonic toothbrush is better than a traditional toothbrush. However, even a powerful sonic toothbrush may not always be enough. In particular, it’s nearly impossible to hit every tooth surface at exactly the right 45-degree angle to your gum line.
New technology has come out utilizing three distinct toothbrush heads working at teeth from three different angles at once.
Multiple studies have concluded that triple-headed toothbrushes show promise for efficiently removing plaque which may otherwise drive inflammation seen in periodontitis.
A recent systematic review revealed that triple-headed toothbrushes worked marginally better than single-headed toothbrushes when a person brushed their own teeth. But the triple-headed one was significantly more effective at plaque removal when a caregiver brushed a person’s teeth.
A 2011 study almost makes you chuckle. Though a dentist was able to effectively brush a child’s teeth with both a conventional and a triple-headed toothbrush, while a child’s mother had more success removing plaque with a triple-headed toothbrush.
Delivering a superior clean in under half the time seems like a no brainer. The right brush is your best defense against periodontitis!
Medical Treatments for Gum Disease
Is periodontitis reversible? Early stages of periodontitis are reversible with good oral hygiene practices.
But in the more advanced stages of gum disease, only a dentist/periodontist may be able to treat your periodontitis.
In any case, you should visit your dental hygienist at least twice a year for your checkup, so they can perform a professional cleaning.
To diagnose periodontitis, your dentist may use dental X-rays to spot bone loss or, as I mentioned earlier, a periodontal probe.
If you have gum disease, a dentist will discuss your options with you:
- Antibiotics may be prescribed to deal with the trickier bacterial infections that professional cleanings have not curtailed. The antibiotics could be in the shape of a mouthwash, gel, or an oral medication.
- Beyond a simple biannual professional cleaning, you may need a little deeper clean:
- Scaling eliminates dental plaque and tartar, all the way into the periodontal pocket.
- Root planing smooths out your teeth, getting rid of tough spots where bacteria like to gather. Root planing also helps gums reattach to your teeth.
- Surgery may need to occur:
- Flap surgery — Under sedation, a dental surgeon will lift up your gums, deep clean your tooth roots, then stitch your gums back where they belong.
- Bone grafting — If you have experienced bone loss, you may need bone grafting. This can be performed at the same time as a flap surgery.
Periodontitis Statistics
- The US Centers for Disease Control estimate more than 47% of American adults have periodontal disease, whether they know it or not.
- Seven out of ten adults with gum disease were aged 65 plus.
- Men are more likely than women to have periodontitis — 56% versus 38%.
- Periodontitis is the most common cause of tooth loss.
- Moderate to advanced gum disease is most common in the Hispanic and black populations.
- New Mexico has the highest prevalence of gum disease. Utah has the lowest.
- 30% of people develop periodontitis because of genetics.
In Summary
Periodontitis is, simply put, gum disease. As bacteria turns into plaque, your gums begin to inflame and recede, which may eventually lead to bone loss and painful sensitivity.
The four stages of periodontitis are:
- Gingivitis — gum inflammation, swelling
- Early — gum bleeding, bad breath
- Moderate — loose teeth, increased sensitivity
- Advanced — loss of teeth
Symptoms of periodontitis include bleeding, red, or tender gums, bad breath, receding gums, tooth and/or bone loss, among others.
You can reverse gingivitis if you:
- Brush at a 45 degree angle towards your gums.
- Brush gently, and in a circular motion.
- Brush your teeth for at least two minutes.
- Use a sonic (or, electric) toothbrush, preferably with a three-sided toothbrush head.
- Floss every day.
- Scrape your tongue every day.
- Don’t use tobacco products.
- Use oral probiotics.
How can my dentist treat periodontal disease?
- Professional cleaning
- Antibiotics
- Scaling, root planing
- Flap surgery, bone grafts
Sources
- Dean, R. (2017). The Periodontal Ligament: Development, Anatomy and Function. King’s College, 1, 1-7. Full text: https://www.longdom.org/open-access/the-periodontal-ligament-development-anatomy-and-function.pdf
- Cepeda, M. S., Weinstein, R., Blacketer, C., & Lynch, M. C. (2017). Association of flossing/inter?dental cleaning and periodontitis in adults. Journal of clinical periodontology, 44(9), 866-871. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5601277/
- Jain, Y. (2013). A comparison of the efficacy of powered and manual toothbrushes in controlling plaque and gingivitis: a clinical study. Clinical, cosmetic and investigational dentistry, 5, 3. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3652371/
- Kulkarni, P., Singh, D. K., & Jalaluddin, M. (2017). Comparison of efficacy of manual and powered toothbrushes in plaque control and gingival inflammation: A clinical study among the population of East Indian Region. Journal of International Society of Preventive & Community Dentistry, 7(4), 168. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5558249/
- Borojevic, T. (2012). Smoking and periodontal disease. Materia socio-medica, 24(4), 274. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3633395/
- Alkhatib, M. N., Holt, R. D., & Bedi, R. (2005). Smoking and tooth discolouration: findings from a national cross-sectional study. BMC Public Health, 5(1), 27. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1079878/
- Worthington, H. V., MacDonald, L., Pericic, T. P., Sambunjak, D., Johnson, T. M., Imai, P., & Clarkson, J. E. (2019). Home use of interdental cleaning devices, in addition to toothbrushing, for preventing and controlling periodontal diseases and dental caries. Cochrane Database of Systematic Reviews, (4). Abstract: https://www.ncbi.nlm.nih.gov/pubmed/30968949
- Fleming, E. B., Nguyen, D., Afful, J., Carroll, M. D., & Woods, P. D. (2018). Prevalence of daily flossing among adults by selected risk factors for periodontal disease—United States, 2011–2014. Journal of periodontology, 89(8), 933-939. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6434526/
- Quirynen, M., Avontroodt, P., Soers, C., Zhao, H., Pauwels, M., & Van Steenberghe, D. (2004). Impact of tongue cleansers on microbial load and taste. Journal of clinical periodontology, 31(7), 506-510. Abstract: https://onlinelibrary.wiley.com/doi/abs/10.1111/j.0303-6979.2004.00507.x
- Almas, K., Al-Sanawi, E., & Al-Shahrani, B. (2005). The effect of tongue scraper on mutans streptococci and lactobacilli in patients with caries and periodontal disease. Odonto-stomatologie tropicale= Tropical dental journal, 28(109), 5-10. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/16032940
- Pedrazzi, V., Sato, S., de Mattos, M. D. G. C., Lara, E. H. G., & Panzeri, H. (2004). Tongue?cleaning methods: a comparative clinical trial employing a toothbrush and a tongue scraper. Journal of periodontology, 75(7), 1009-1012. Abstract: https://aap.onlinelibrary.wiley.com/doi/abs/10.1902/jop.2004.75.7.1009?rfr_dat=cr_pub%3Dpubmed&rfr_id=ori%3Arid%3Acrossref.org&url_ver=Z39.88-2003
- Lussi, A., Jaeggi, T., & Zero, D. (2004). The role of diet in the aetiology of dental erosion. Caries research, 38(Suppl. 1), 34-44. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/14685022
- Shanbhag, V. K. L. (2017). Oil pulling for maintaining oral hygiene–A review. Journal of traditional and complementary medicine, 7(1), 106-109. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5198813/
- Seminario-Amez, M., López-López, J., Estrugo-Devesa, A., Ayuso-Montero, R., & Jané-Salas, E. (2017). Probiotics and oral health: A systematic review. Medicina oral, patologia oral y cirugia bucal, 22(3), e282. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5432076/
- Mahasneh, S., & Mahasneh, A. (2017). Probiotics: A promising role in dental health. Dentistry journal, 5(4), 26. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5806962/
- Azrak, B., Barfaraz, B., Krieter, G., & Willershausen, B. (2004). Effectiveness of a three-headed toothbrush in pre-school children. Oral health & preventive dentistry, 2(2). Abstract: https://www.ncbi.nlm.nih.gov/pubmed/15646943
- Ashkenazi, M., Salem, N. F., Garon, S., & Levin, L. (2015). Evaluation of Orthodontic and Triple-headed Toothbrushes When Used Alone or in Conjunction with Single-tufted Toothbrush in Patients with Fixed Lingual Orthodontic Appliances. A Randomized Clinical Trial. The New York state dental journal, 81(3), 31-37. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/26094361
- Kalf?Scholte, S. M., Van der Weijden, G. A., Bakker, E. W. P., & Slot, D. E. (2018). Plaque removal with triple?headed vs single?headed manual toothbrushes—a systematic review—. International journal of dental hygiene, 16(1), 13-23. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/28544459
- Oliveira, L. B., Zardetto, C. G. D. C., de Oliveira Rocha, R., Rodrigues, C. R. M. D., & Wanderley, M. T. (2011). Effectiveness of triple-headed toothbrushes and the influence of the person who performs the toothbrushing on biofilm removal. Oral health & preventive dentistry, 9(2). Abstract: https://www.ncbi.nlm.nih.gov/pubmed/21842016